Diabetes is a disease affecting the insulin producing glands, characterized by the body’s inability to produce or effectively utilize insulin, a hormone that regulates blood glucose levels. This condition leads to a range of symptoms, including hyperglycemia, polyuria, and polydipsia, and can have severe health implications if left untreated.
The mechanisms underlying diabetes involve insulin resistance and beta-cell dysfunction, leading to impaired glucose metabolism. Understanding the pathophysiology, symptoms, and complications of diabetes is crucial for effective management and prevention.
Pathophysiology of Diabetes
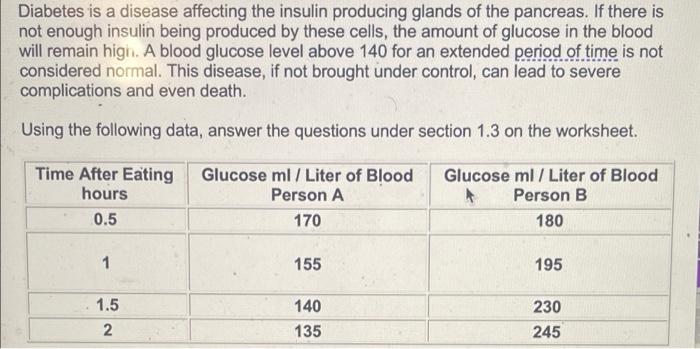
Diabetes is a chronic metabolic disorder characterized by elevated blood glucose levels. Insulin, a hormone produced by the beta cells of the pancreas, plays a crucial role in glucose metabolism by facilitating its uptake into cells for energy production.
Insulin Resistance and Beta-Cell Dysfunction
In diabetes, insulin resistance occurs when cells become less responsive to insulin, leading to impaired glucose uptake. This resistance can result from genetic factors, obesity, physical inactivity, and certain medications.
Beta-cell dysfunction, the other key factor in diabetes, involves the inability of the pancreas to produce sufficient insulin to overcome insulin resistance. This dysfunction can be caused by autoimmune destruction of beta cells (type 1 diabetes) or gradual decline in their function (type 2 diabetes).
Types of Diabetes
- Type 1 Diabetes:An autoimmune disease in which the immune system attacks and destroys beta cells, leading to an absolute deficiency of insulin.
- Type 2 Diabetes:The most common type, characterized by insulin resistance and progressive beta-cell dysfunction. Obesity, physical inactivity, and family history are major risk factors.
- Gestational Diabetes:A temporary form of diabetes that occurs during pregnancy due to hormonal changes that interfere with insulin action.
Symptoms and Diagnosis of Diabetes
Common symptoms of diabetes include:
- Hyperglycemia (high blood glucose levels)
- Polyuria (excessive urination)
- Polydipsia (excessive thirst)
- Unexplained weight loss
- Fatigue
- Blurred vision
Diagnostic Criteria
Diabetes is diagnosed based on the following criteria:
- Fasting plasma glucose ≥ 126 mg/dL (7.0 mmol/L)
- Oral glucose tolerance test: 2-hour plasma glucose ≥ 200 mg/dL (11.1 mmol/L)
- HbA1c ≥ 6.5% (48 mmol/mol)
Importance of Early Diagnosis
Early diagnosis and treatment of diabetes are crucial to prevent complications and improve overall health outcomes.
Complications of Diabetes
Diabetes can lead to both acute and chronic complications:
Acute Complications
- Diabetic ketoacidosis (DKA):A life-threatening condition caused by severe insulin deficiency, leading to ketoacidosis.
- Hyperosmolar hyperglycemic nonketotic syndrome (HHNS):Another life-threatening condition characterized by extremely high blood glucose levels without ketoacidosis.
Chronic Complications
Long-term complications of diabetes include:
- Cardiovascular disease:Diabetes increases the risk of heart disease, stroke, and peripheral artery disease.
- Nephropathy:Damage to the kidneys, leading to proteinuria and potentially kidney failure.
- Retinopathy:Damage to the blood vessels in the retina, which can lead to blindness.
- Neuropathy:Nerve damage, which can cause pain, numbness, and weakness in the feet and hands.
Prevention of Complications
Managing blood glucose levels within the target range is essential to prevent or delay the development of complications.
Treatment and Management of Diabetes

Treatment options for diabetes include:
Insulin Therapy
Insulin injections are used to replace or supplement the body’s own insulin production.
Oral Medications
Various oral medications are available to improve insulin sensitivity, increase insulin secretion, or reduce glucose absorption.
Lifestyle Modifications, Diabetes is a disease affecting the insulin producing glands
Lifestyle modifications, including:
- Healthy diet
- Regular exercise
- Weight management
are essential for effective diabetes management.
Regular Monitoring and Self-Care
Regular blood glucose monitoring and self-care practices, such as foot care and medication adherence, are crucial for managing diabetes effectively.
Prevention and Public Health Implications

Risk factors for diabetes include:
- Obesity
- Physical inactivity
- Family history
Prevention Strategies
Preventing diabetes involves:
- Promoting healthy lifestyles
- Early detection and intervention
Public Health Implications
Diabetes has a significant public health impact, with its prevalence and economic burden increasing globally.
Helpful Answers: Diabetes Is A Disease Affecting The Insulin Producing Glands
What are the common symptoms of diabetes?
Common symptoms include excessive thirst, frequent urination, unexplained weight loss, increased hunger, and fatigue.
What are the risk factors for developing diabetes?
Risk factors include obesity, physical inactivity, family history, and certain genetic predispositions.
Can diabetes be prevented?
While not all cases can be prevented, maintaining a healthy weight, engaging in regular physical activity, and adopting a balanced diet can significantly reduce the risk.